Be sure to watch all videos on this page
Measuring vital signs and recording these is a very important component in the skills needed in being a C.N.A.
Huge decisions are based on the information you documentation and therefore it must be accurate. Decisions such as medication doses, health status, physical therapy approvals and much more are example of decisions based on your documentation.
Measuring vital signs is a skill that takes time to master. In this class we will teach these skills but you will need to continue to practice to gain proficiency.
Some healthcare setting will use automated machines but these may not always be available and are subject to breaking down, giving inaccurate readings or may not be charged up when needed. If a resident is in isolation or quarantine a personal manual equipment is generally used. For these reasons it is important that learning and becoming proficient in measuring vital signs is important to be considered a professional and to give the best care for your residents.
Temperature
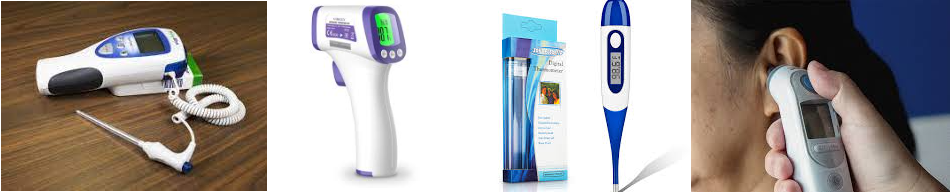
Measuring Temperature
Body temperature is a measure of how well the body can make and get rid of heat. Generally, the body is very good at keeping its temperature within a safe range.
The body strives for homeostasis (balance) in every system and temperature is included.
When the body is too hot, the blood vessels in your skin widen to carry the excess heat to the skin's surface resulting in sweating. As the sweat evaporates, it helps to cool the body.
When the body becomes too cold, the blood vessels constrict to become narrower. This reduces blood flow to the skin to save body heat and shivering can occur. When the muscles tremble (shiver) it creates heat.
Temperature can be measured in many places on the body. The most common locations are the mouth, the ear, the armpit, and the rectum. Temperature can also be measured on your forehead.
The rectum is almost never used any longer in a LTC setting and a glass thermometer is prohibited because of the mercury inside the tube can escape if the tube breaks.
Thermometers show body temperature in either degrees Fahrenheit (°F) or degrees Celsius (°C). In the United States, temperatures are often measured in degrees Fahrenheit, make certain the thermometer you are using is turned on to F not the C.
The main reason for taking a temperature is to check for fever. Please be aware that the immune system must be intact for a person to have a fever. If your resident is immunocompromised, they may be quite ill yet not show much elevation in temperature. This reason is cause to check for other signs of infection such as cough, headache, a general feeling of malaise meaning just feeling weak and ill.
Wait at least 20 minutes after smoking, eating, or drinking fluids or bathing.
The thermometer needs to be clean and generally a sheath or protective covering is used and replaced with every use.
With so many options on the market today, it will be important to learn the type on procedure for the thermometer at your LTC community. Because there are so many only the most common will be reviewed here.
Oral (by mouth) is the most common method of taking a temperature. For you to get an accurate reading, the person must be able to breathe through their nose. If they can't, then use the ear (tympanic- ty), or armpit (axillary- ax), or forehead (temporal- t) to take the temperature. Although the tympanic route is deemed most accurate, many factors can scew results including technique and excessive ear wax. Check as some thermometers can only be used on a particular body location. Leave the thermometer in place for the required amount of time. Many devices will beep when completed.
Before taking a temperature, read the instructions for how to use that type of thermometer.
If oral, place the thermometer under the tongue, just to one side of the center, ask the resident to close their lips tightly around it.
For an axillary temperature place it deep in the armpit and close the arm snuggly over.
Use of the tympanic thermometer, pull gently on the top/side of the ear to straighten the ear canal, insert the probe (it is only about ¼ inch in length) push the button and wait for the beep to signal it is finished.
Record the result noting the type or location of the temperature.
Example: 98.9 Ax refers that the temp was taken under the arm. O is for oral. Ty is usually for tympanic, but do check as policies may vary.
The elderly tend to have slightly lower temperature, and every resident will have their own normal.
Temperature Normal Ranges- one degree below average to one degree above
The normal range for temperatures vary depending on their route. For example, rectal is deeper in the body and runs hotter than most surface temperatures like axillary.
o-Oral- 98.6 (97.6-99.6)
ty-Tympanic- 98.6 (97.6-99.6)
r-Rectal 99.6 (98.6-100.6)
ax- Axillary 97.6 (96.6-98.6)
t- temporal 97.6 (96.6-98.6)
Pulse
Resting heart rate is taken when a calm individual is sitting or lying down. A normal resting heart rate for an adult is between 60-100 bpm (beats per minute). High resting heart rate may be caused by exercise, illness, certain medications, heart disease, and stress. Several medicines can cause low resting heart rate.
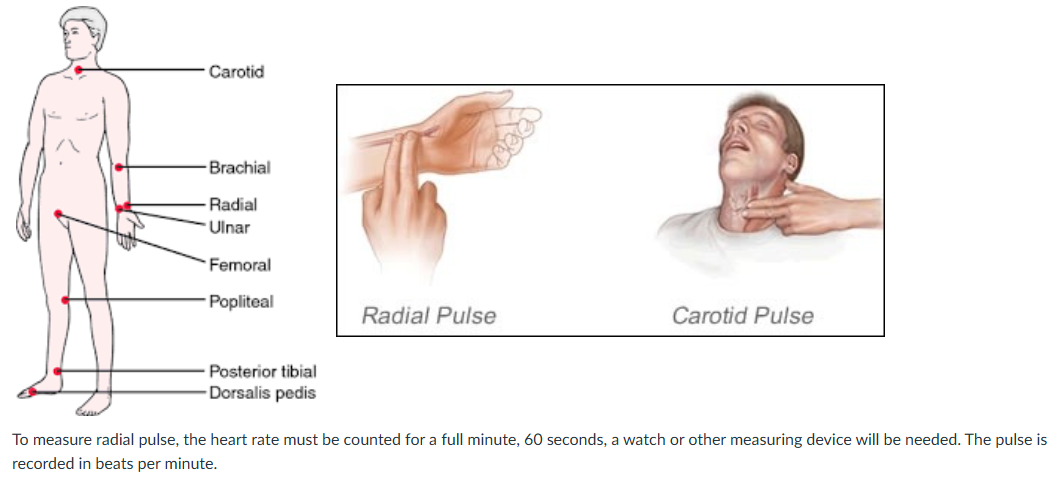
Pulse can be felt through the skin on several location in the body (see the picture below). In this skill we are focusing on measurement of pulse through the radial artery in the wrist, the radial pulse.
Apical Pulse
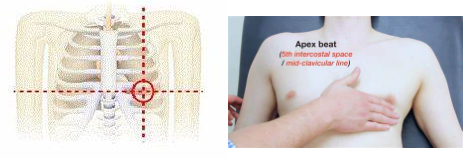
The apical pulse (ap) is taken using a stethoscope and listening to the heart as it beats. The key to taking an apical pulse is finding it. What you actually want to listen to the bottom portion of the heart, the part that appears pointed, otherwise known as the apex of the heart. This is where you can hear it the loudest. It is found on the center of the left side of the chest and about five ribs down from the collar bone. It is heard best when the stethoscope is placed inbetween the ribs. The heart makes two thumps which equals one beat and should always be counted for a full minute.
A rapid pulse rate, above 100, is called Tachycardia
A slow pulse rate below 60 is called Bradycardia
A pulse can be thready or bounding. Thready is a weak pulse that is difficult to palpate (feel with the fingers), a bounding pulse is a hard and forceful pulse and sometimes can be seen through the skin on the neck and other places. A pulse can also be regular or irregular referring to the rhythm. An irregular pulse may need to be repeated for accuracy.
Notify the nurse immediately when a pulse is not within normal limits.
Respirations
When counting respirations, one inhalation, (breathing in) and one exhalation (letting out the breath) counts as 1 respiration.
A normal rate of respiration for adults is 14 to 20 respirations per minute.
Respirations are measured in respirations or breaths per minute.
A count of one full minute, 60 seconds, is required.
When taking a resident's respiration rate make sure they have not just finished walking or exercising, if so wait 20 minutes and return.
Generally respirations are taken immediately after the pulse while still holding the wrist so the person is unaware and breathing is not altered unintentionally.
If you are unable to see the rise and fall of the chest so as to count the respiration, place your hand on the resident's back or shoulder.
A bluish tint to the lips and grey or ashen look to the skin is called cyanosis.
The medical term for fainting is syncope.
Dyspnea is difficulty breathing, labored breathing.
Apnea is the absence of breath for a time as in sleep apnea.
Wheezing is a high pitched whistling sound when breathing usually associated with asthma.
Contact the nurse immediately if respirations are irregular or labored.