Catheters
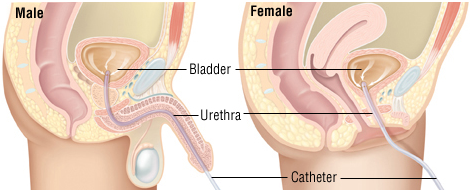
For certain resident situations, devices are placed to collect urine. A catheter is a thin tube inserted into the body that is used to drain fluids or inject fluids. A straight catheter is a type of catheter that is inserted to drain urine from the bladder. It is removed immediately after urine is drained. It does not remain inside the person.
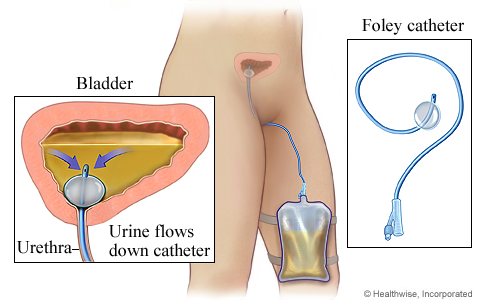
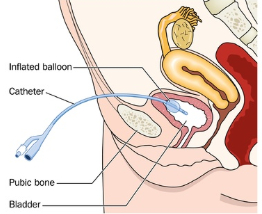
An indwelling catheter (also called a Foley catheter) remains inside the bladder for a period of time. Urine flows through the tube and the catheter is held in place within the bladder by a small inflated balloon at the tube’s tip. A catheter is connected to drainage tubing and a collection bag.
The interior of the catheter, tubing, and bag is considered sterile. The use of a catheter greatly increases the risk for urinary tract infections and other systemic infections. Restorative goals are aimed at helping a resident return to normal bladder function and control of elimination.
Another type of catheter is a suprapubic catheter. This is a retention catheter inserted into the bladder through a surgical opening in the abdomen.
The condom catheter (also called the Texas catheter) is used for males. It has an attachment on the end that fits onto the penis and is fastened with special tape. Urine drains through the catheter into the tubing, then into the drainage bag.
CNA's responsibilities:
Wash and dry penis
If resident is not circumcised, place foreskin in normal (non-retracted) position.
Roll catheter sheath over penis, leaving 1” space at tip.
Use elastic adhesive tape provided with external catheter to secure to penis. Apply in spiral
pattern, tight enough to prevent leakage but loose enough to allow blood circulation to tissue.Re-apply daily or when leaking.
Observations:
Observe for skin irritation
Observe for leaking of system
Collection bags
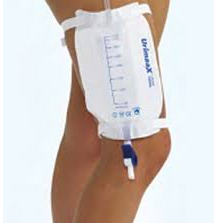
Large capacity collection bags are usually positioned away from the body on either a floor stand or a hanger that hooks onto a bed or chair frame. They are commonly called night bags.
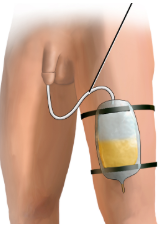
A leg drainage bag is a small collection bag that can be strapped to the resident’s leg, under clothing. This is less visible than the larger bag, but holds less volume. Leg drainage bags must be emptied more frequently.
CNA's responsibilities:
Understand that inserting a catheter is the responsibility of the nurse.
Understand urinary elimination goals that are part of the resident’s care plan.
Position catheter with no tension on the urethra. Facility protocols may allow the use of a strap to support the tubing on the resident’s upper thigh.
Protect tubing from kinks and pressure. Protect tubing while resident changes position or ambulates.
Position tubing to allow for gravity drainage. Keep drainage bag lower than bladder to prevent backflow. Never lay the bag on the floor.
Position bag out of public view, if resident prefers. A cloth bag “cover” may be used to shield from view.
Prevent introduction of organisms that can cause infection. Maintain sterile connections whenever system is opened.
Disconnect/reconnect catheter from drainage system only when task is directed by supervising nurse. The nurse will verify that CNA can maintain sterile connections.
Follow facility protocol for replacing drainage bags. Leg bag may be replaced each day or disinfected between uses.
Emptying drainage bag -Using knowledge of infection control measures, follow techniques describes in nursing skills text. Common points include:
Maintain sterility of system by careful handling of drainage spout and bag.
Empty into graduated measuring cup according to facility policy, often every eight hours. Measure and record output.
Observe urine for abnormal color and clarity.
Dispose of urine in toilet.
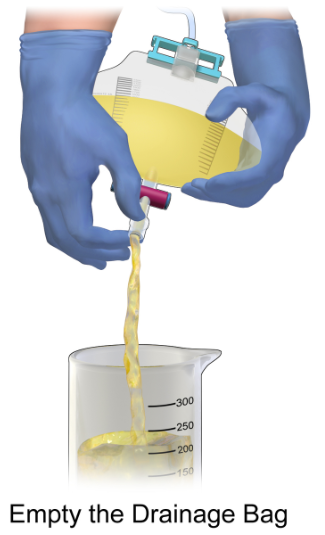
Emptying the Catheter Drainage Bag
Wash your hands.
Explain the procedure to the resident.
Provide privacy.
Put on gloves.
Place a paper towel on the floor under the drainage bag. Place the measuring cup on the paper towel.
Open the clamp on the bag so that urine flows out of the bag and into the measuring cup. Do not let the spout or clamp touch the cup.
When the urine has drained from the bag, close the clamp. Using alcohol wipes, clean the drain spout. Place the drain spout back in its holder on the bag.
Go into the bathroom. Place graduate on a flat surface and measure at eye level. Note the amount and characteristics of urine. Empty into the toilet and flush the toilet.
Clean and store measuring cup or device. Discard paper towels.
Remove and discard gloves.
Wash your hands.
Document procedure using facility guidelines. Note amount and characteristic's of urine.
Routine Catheter Care
CNA's do not insert, remove, or irrigate catheters. CNA's may be asked to give daily catheter care, clean the area around urethral opening, and empty the drainage bag. Keeping the genital area clean helps prevent infection. Because the catheter goes all the way into the bladder, bacteria can enter the bladder more easily. Daily care of the genital area (perineal care) is especially important.
Thoroughly wash your hands before giving catheter care.
Explain the procedure to the resident. Speak clearly, slowly and directly. Maintain face-to-face contact whenever possible. (Promotes understanding and independence.)
Provide privacy
Adjust the bed to a safe level, usually waist high, Lock bed wheels. (This helps prevents injury)
Lower the head of the bed. Position the resident lying flat on her back.
Remove or fold back top bedding. Keep the resident covered with a bath blanket.
Test the water temperature with the inside of your wrist. Water should be no higher than 105 degree F. Have the resident check the water temperature and adjust if needed.
Put on gloves.
Ask the resident to flex their knees and raise their buttocks off the bed by pushing against the mattress with their feet. Place clean bed protector under their perineal area, including their buttocks.
Expose only the area necessary to clean the catheter. Avoid overexposing the resident.
Place a towel under the catheter tubing before washing. (Helps keep bedding from getting wet.)
Wet a washcloth in the basin. Apply soap to the washcloth. Clean the area around the meatus (opening to the urethra) and avoid tugging the catheter.
Clean at least four inches of the catheter nearest to the meatus. Move in only one direction, away from the meatus. Use a clean area of the washcloth for each stroke.
Dip a clean washcloth in the water. Rinse area around the meatus, using a clean area of the washcloth for each stroke. With a clean, dry towel, dry the area around the meatus.
With a clean, dry towel, dry at least four inches of catheter nearest to the meatus. Move in only one direction, away from the meatus. Do not tug the catheter.
Remove bed protector from under resident and discard. Remove towel from under the catheter tubing and place in proper container. Replace top top covers. Remove bath blanket and place in proper container.
Place used washcloths in proper container.
Empty the basin into the toilet and flush the toilet. Place basin in proper area for cleaning or clean and store it according to facility policy.
Remove and discard gloves.
Wash your hands.
Return bed to lowest position.
Place call light within resident's each.
Report any changes in resident to the nurse.
Document procedure using facility guidelines.
Make sure that the drainage bag always hangs lower than the hips or bladder. Urine must never flow from the bag or tubing back into the bladder. This can cause infection.
Keep the drainage bag off the floor. Make sure the catheter tubing does not touch the floor.
Keep the tubing as straight as possible. It should not be kinked.
Observations
Notify nurse promptly of any potential problem!
Observe color, clarity, and odor of urine. (Urine should be light yellow, clear, and nearly odorless.)
Report if there is blood in the urine
Report if odor is present
Observe for continuing flow of urine. Check every few hours.
Report if catheter bags does not fill after several hours or if the bag fills suddenly
Observe for leaking of system or leaking from urethra.
Observe for perineal redness or irritation.
Observe for indications of pain (verbal report or nonverbal behavior).