Pain is sometimes refered to as the sixth vital sign. Pain is common amongst the geriatric population and should be screened for. Chronic pain can lead to anxiety, depression, fatigue, and insomnia. Whether it be aching joints from osteoarthritis, a throbbing tooth, or inflammation from disease or infection, the elderly tend to have their fair share. Often pain goes undetected in this population as many believe they are old and pain is normal and there is nothing that can be done to stop it. Often, they trudge through it without complaint. Other chronic issues can make it difficult if not impossible for residents to communicate pain or in the case of dementia, they may not recognize they are in pain. Therefore, it is very important that caregivers know how to recognize pain and report it.
Dementia
Most residents show pain through grimacing, groaning, hesitation, limping, frowning, or crying. Most can tell you they have pain. Residents with dementia, however, may not even recognize they are in pain. They often show they are in pain by becoming excessively anxious, pacing, or combative. When asked if they have pain they might deny it, and yet, after pain management is implemented, they suddenly calm down. Experts say this is because they feel pain but cannot process this in their brains. They know something is wrong, but don’t know what or why, and this can lead to increased confusion and agitation seen in dementia patients in pain.
Role as a CNA
CNA’s are not responsible for assessing pain, that is the nurse’s job. But it is very important that the CNA recognizes pain and has an attitude that pain can be treated, and should be treated. As a CNA watch for signs of pain and report them to the nurse. Additionally, the nurse may have you implement pain management techniques such as:
Repositioning
Heat therapy
Cold therapy
Elevation
Massage
Pain Scales
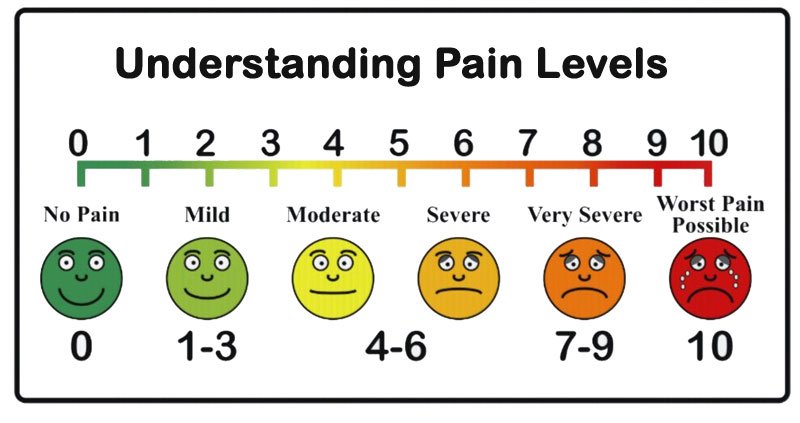
Some facilities use pain scales to help screen for pain. There are many different kinds that can be used. The 0-10 pain scale is most popular. You ask the resident, “On a scale from 0-10, 10 being the worst pain you can imagine, where would you rate your pain?” On this scale, mild pain would be 1-3, moderate pain 4-6, and severe pain would be 7-10. NOTE: pain is what the patient says it is. People experience pain and deal with pain differently. Try not to be judgmental about their response. Just because someone may not look like they have pain 10/10, if that is what they say it is, then that is what it is and that is what should be reported and documented.
Because it can be very difficult to put a number to their pain, sometimes a Faces Scale is used to determine pain level. In this scale, you can ask them which face best describes how they feel. Remember that it may not be the expression they are making at the time as they may be trying to be strong and are hiding their pain.